About the Report
The use of medicines in the United States is a critical factor influencing the health outcomes of millions of Americans. This report provides objective measures of medicine use and its costs to the U.S. healthcare system and patients, employers, health plans, intermediaries and state and federal government agencies.
The report specifically focuses on the volume of medicine use – with a special attention on opioids – drivers of change in the use of medicines, overall “net spending,” out-of-pocket costs to patients, and an outlook through 2023 for the pharmaceuticals market. It additionally examines the key dynamics around new product launches, patent expiries and the introduction of generics and biosimilars.
Report Summary
Medicine use has continued to rise, with Americans filling 5.8 billion prescriptions in 2018, a gain of 2.7% over the prior year. At the same time, prescription opioid volumes have declined by 43% since their peak in 2011, with the most potent and dangerous high-dose prescriptions declining by 61% over the same period. The use of specialty medicines grew by 5%, more than twice the rate of other drugs, and now represents 2.2% of volume.
In 2018, medicines spending growth in the United States rebounded to 4.5% on a net basis, while growth at the invoice-level was 5.7%. Net medicine spending was $1,044 per person, up 0.9% or $10 from 2017. Total net spending growth in 2018 was largely driven by more patients receiving existing branded drugs and using newly launched drugs.
In aggregate, patient out-of-pocket costs climbed in 2018 to an estimated $61 billion. Across all pay types, 8.8% of patients pay more than $500 for prescriptions. Commercially insured patients increasingly use manufacturer coupons to offset their initial cost exposure, and average final out-of-pocket costs remained at $42 per brand prescription.
The base case outlook in the next five years forecasts that net medicine spending in the United States will increase from $344 billion in 2018 to $420 billion in 2023, an aggregate growth of $76 billion and lower than the $84 billion growth seen over the past five years. The largest driver of this growth will be the launch of new branded drugs.
A number of policy changes are currently under consideration, and this report examines alternative forecast scenarios based on their impact on various attributes and stakeholders. In a scenario where reforms are limited to Medicare programs, out-of-pocket costs decline $14 billion and net spending decreases by as much as 6%. In another scenario, if reforms proposed for Medicare are extended to the commercial market, out-of-pocket costs would decline by 30% and drive net spending 9% lower than base case projections.
Key Findings
Americans are taking more prescription medicines: there were 5.8 billion prescriptions dispensed in the United States in 2018, up 2.7% from 2017
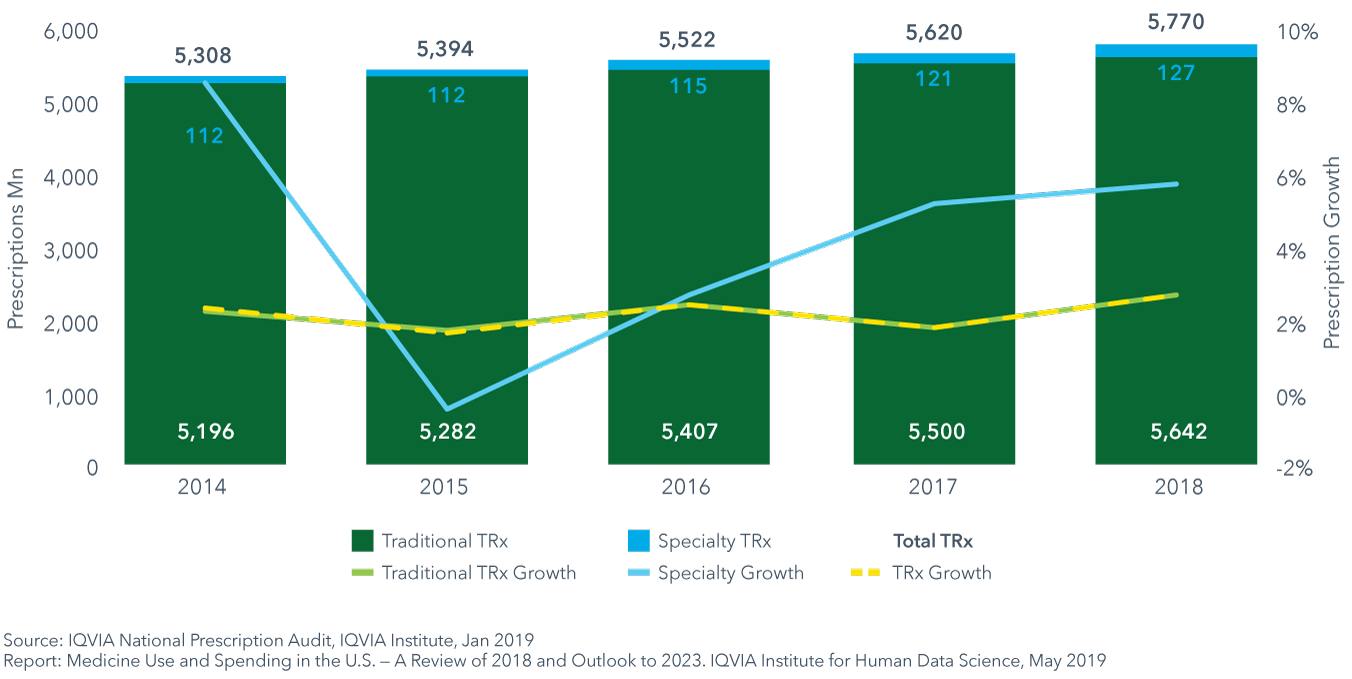
- In total, 127 million specialty prescriptions were dispensed in retail and mail pharmacies in 2018, up by 15 million since 2014.
- Specialty medicine prescriptions grew by over 5% even as those medicines account for only 2.2% of prescriptions and have little impact on the overall growth of dispensed prescriptions.
- Chronic prescriptions account for more than two-thirds of prescriptions, and the increasing use of 90-day prescriptions means patients have significantly more medicine on hand.
2018 saw the steepest drop in opioid prescription use – down 17.1% from 2017 levels
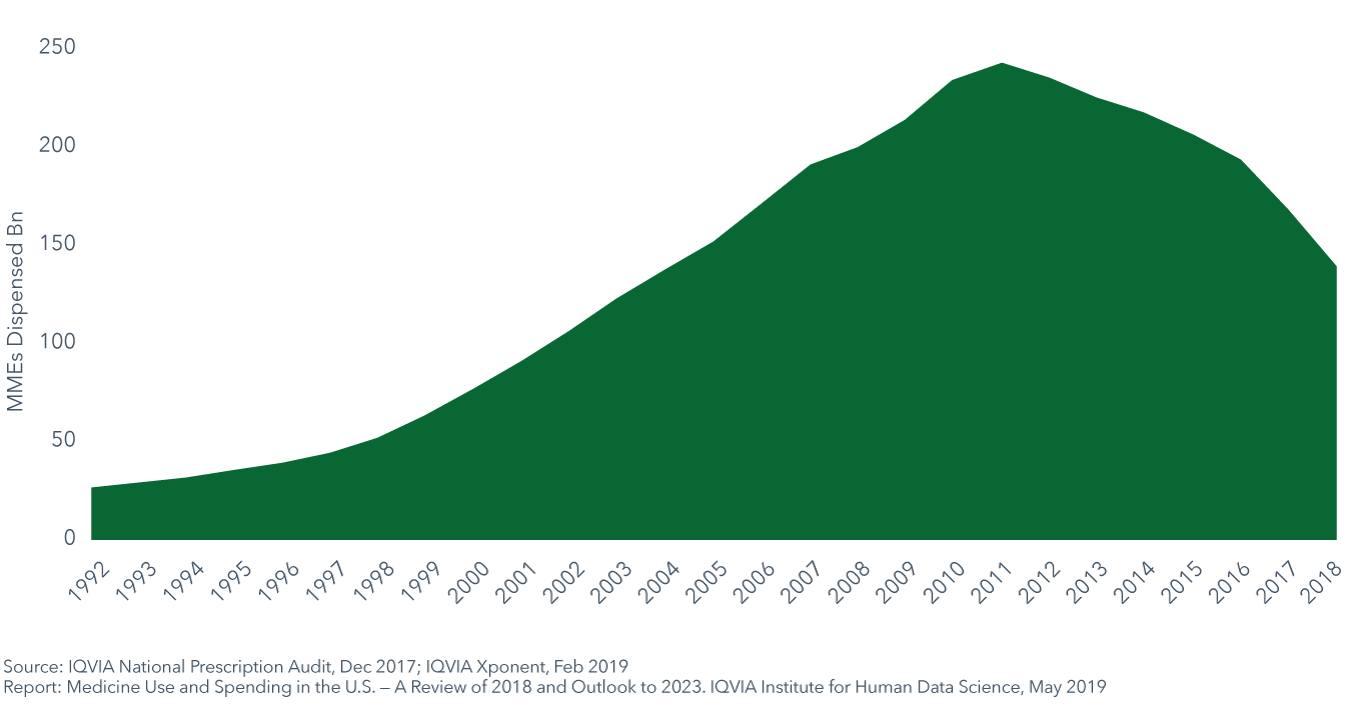
- 2018 saw the largest single-year decline in prescription opioid volume, dropping by 29.2 billion morphine milligram equivalents (MME).
- Overall opioid volumes in MME have declined by 43% since the peak in 2011, while prescriptions for 90 MMEs per day or greater declined by 61%.
- Decreases in prescription opioid volume have been driven by changes in clinical use, regulatory and reimbursement policies and legislation that has been increasingly restricting prescription opioid use since 2012.
Real net per capita spending grew by only $44 per person per year since 2009, as specialty drug spending nearly doubled and traditional spending declined
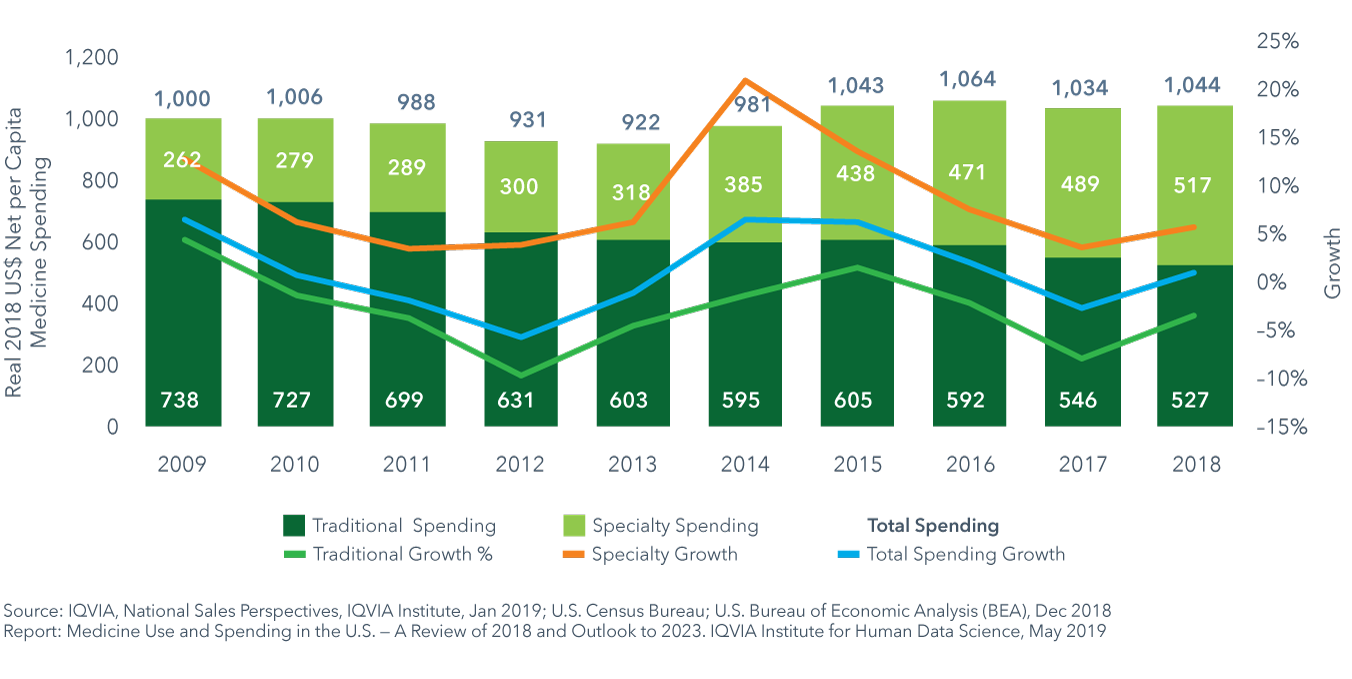
- Net price increases on branded drugs averaged only 0.3% in 2018.
- Real net per capita spending grew by 0.9% from $1,034 per person in 2017 to $1,044 in 2018, and by a 1.1% 10-year CAGR to 2018.
- Net spending on specialty medicines increased 5.8% on a per capita basis, while traditional medicine costs fell 3.4%.
Patient out-of-pocket costs are estimated at $61 billion in aggregate in 2018 – up $2 billion over 2017
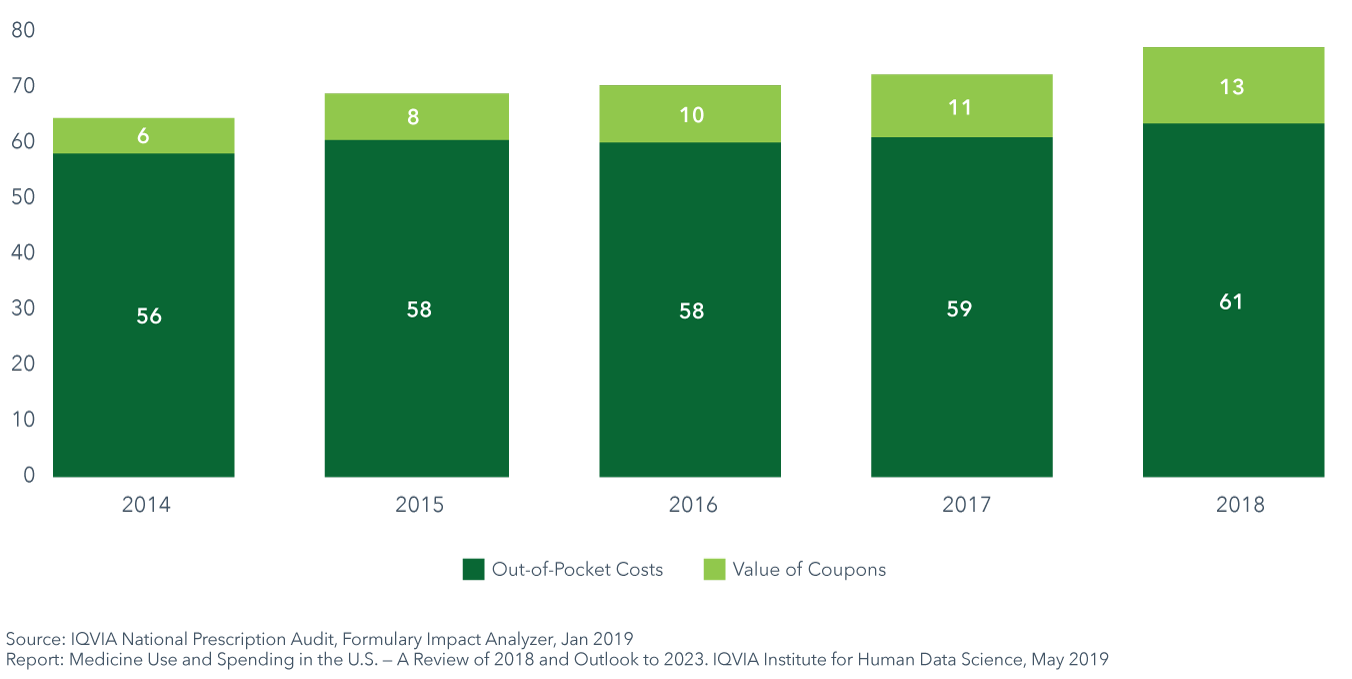
- Overall out-of-pocket costs have risen from $56 billion in 2014 to $61 billion in 2018 although some patients have seen their costs decline as generic prescription costs decline.
- As out-of-pocket costs have risen, $13 billion of costs have been offset by coupons for commercially insured patients.
- Of commercially insured patients on branded medications, 19% of them used coupons to reduce their out-of-pocket costs in 2018.
The potential impact in 2023 of pricing reform scenarios on key metrics relative to the 2018 baseline are substantial
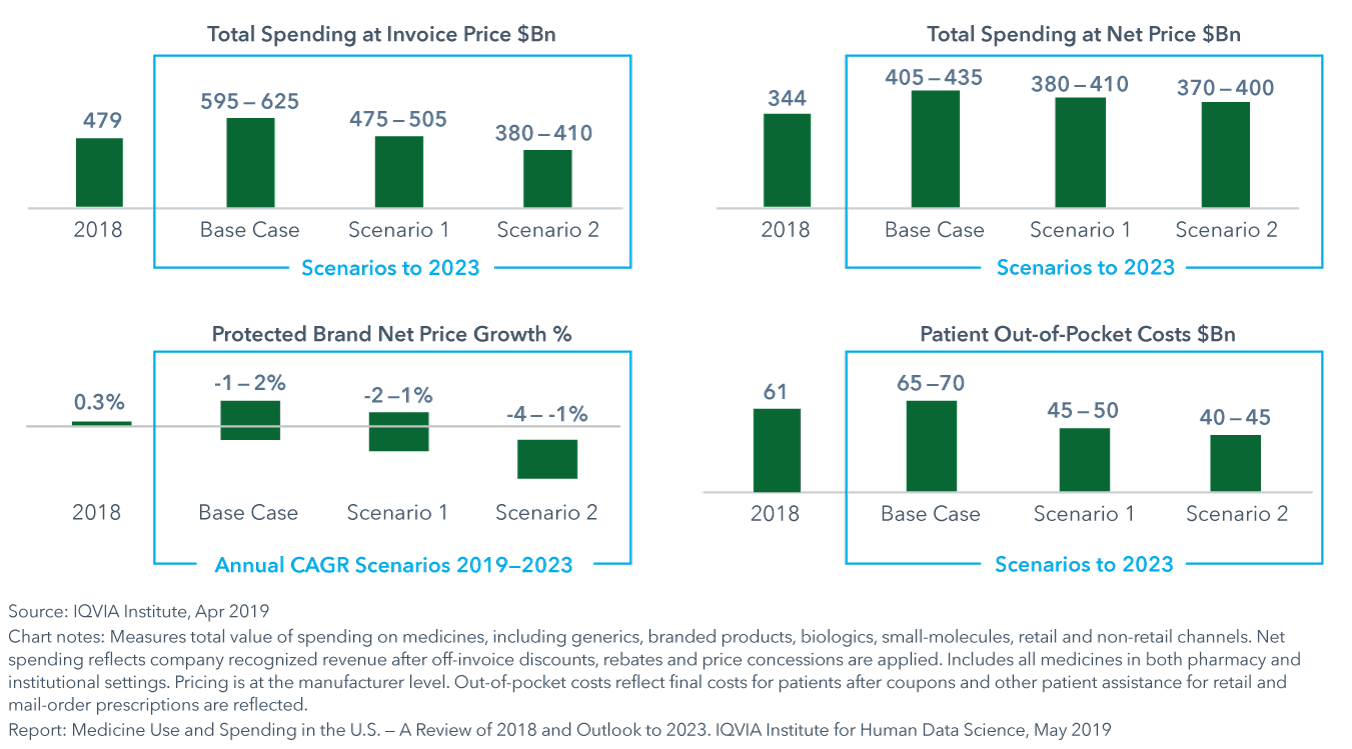
- Potential policy changes could lead to alternative scenarios and impact invoice spending, net spending and out-of-pocket costs in very different ways.
- In one scenario, reforms are limited to Medicare programs, leading to a decline in out-of-pocket costs of $14 billion over the base case and a reduction in net spending by as much as 6%.
- In another scenario, reforms proposed for Medicare would be extended to the commercial market. This could lower out-of-pocket costs 30% and drive net spending 9% lower than base case projections.
Learn More
Use of Medicines in the U.S. A Review of 2018 and Outlook to 2023
Access an on-demand webinar where Michael Kleinrock, report author and Institute Research Director, delves deeper into report findings.